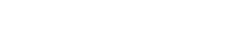Psoriasis


What is Psoriasis?
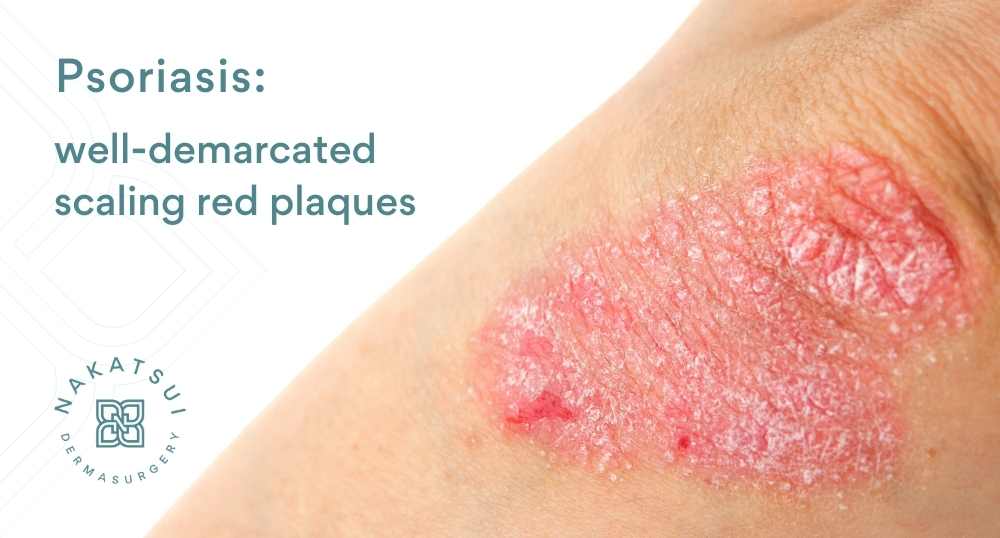
Psoriasis is a skin condition characterized by scaly, red, well-defined plaques scattered over the body. Some of the typical locations are the scalp, elbows, and knees, although it can occur in many different locations on the body, such as the nails, lower back, and genitals. Frequently, it also occurs in a symmetric distribution. It is a very common condition, affecting approximately 3% of the general population. In other words, 3 out of every 100 people you meet in Edmonton has psoriasis, which means a lot of people in Edmonton have this skin condition.
What Causes Psoriasis?
This a great question. There is a very strong immune system component to this condition. In normal skin, the skin cells turn over every 28 days but in psoriasis, the skin cells turn over every 3-4 days. The reason for this is that the immune system is stimulating the growth of skin cells and causes inflammation.
What are Some of the Different Types of Psoriasis?
There are several different types beyond the typical plaque type. One of the variants is guttate psoriasis, which consists of tiny scattered areas typically brought on by a strep throat infection, Another variant is called pustular psoriasis where a person will develop small pustules scattered over the skin, including the palms and soles.
Psoriasis also frequently affects the nails. The increased growth rate of the cells prevents the nail plate from maturing correctly so that small areas fall off causing a pitted appearance to the nails.
Is Psoriasis related to Any Other Health Conditions?
People with this kin condition do have a higher risk of developing other conditions, such as arthritis, high blood pressure (hypertension), cardiovascular disease, diabetes, and depression.

Psoriasis is not infectious. You cannot catch it from someone who has it and you cannot pass it on to someone else.
How to Cure Psoriasis?
Unfortunately, there is still no cure for this skin condition. Even though there is no cure, psoriasis treatments have come a long way and for patients with severe disease, there have been some great advancements in the last decade. If you have been suffering from psoriasis, you should consult a dermatologist here in Edmonton and find out if you are a candidate for one of the newer medications available for this skin condition.
How to Treat Psoriasis
Treatments can be broken down into general measures, topical therapies, light therapy, and systemic therapies. General measures includes using moisturizers to lock in moisture, stop smoking, and decrease alcohol intake to minimize some of the triggers.
Topical therapies come in the form of creams, gels, lotions, and shampoos. They primarily consist of topical steroids, Vitamin D analogues (including Dovonex, Dovobet, and Enstilar), and tar agents. Light therapy includes PUVA, broad band UVB, and narrow band UVB.
Systemic therapies can be divided into oral agents and injectable agent. Oral agents include methotrexate, acitretin (Soriatane), and apremilast (Otezla). Otezla is one of the newest oral medications and has been approved for the treatment of moderate to severe disease and active psoriatic arthritis. It does not have many side effects, although it can cause weight loss and other mild symptoms.

The newest treatments are injectable agents that are in the category of biologic agents. These are medications that interfere with very specific aspects of the immune system. They include:
- TNF-alpha inhibitors such as Remicade or Inflectra (infliximab), Enbrel (etanercept), and Humira (adalimumab)
- IL-12/23 inhibitors such as Stelara (ustekinumab). One of the advantages of Stelara is that it only requires one treatment every 3 months!
- IL-17 inhibitors such as Cosentyx (secukinumab) and Taltz (ixekizumab).
- IL-23 inhibitors such as risankizumab (Skyrizi), tildrakizumab (Ilumya), and guselkumab (Tremfya)
If you have concerns about your psoriasis, you should speak with a dermatologist. You can find a list of Edmonton dermatologists on our home page under “How Do I Know If My Doctor is a Dermatologist?”
FAQs on Psoriasis
How long have biologic agents for psoriasis been around?
Biologic agents have actually been around for many years now even though many psoriasis patients have never heard of them. Some of the first ones are no longer around like Amevive and Raptiva. Here is a list of the agents and the year they were introduced.
- 2003 alefacept (Amevive)
- 2003 efalizumab (Raptiva)
- 2004 etanercept (Enbrel)
- 2006 infliximab (Remicade)
- 2008 adalimumab (Humira)
- 2009 ustekinumab (Stelara)
- 2015 secukinumab (Cosentyx)
- 2016 ixekizumab (Taltz)
- 2017 brodalumab (Siliq)
- 2017 guselkumab (Tremfya)
- 2019 rizankizumab (Skyrizi)
- 2019 certolizumab pegol (Cimzia)
What is TNF-Inhibitor Induced Psoriasis?
TNF inhibitors such as Humira, Enbrel, and Remicade have been commonly used to treat psoriasis. They have also been used to treat other conditions such as rheumatoid arthritis, inflammatory bowel disease, and ankylosing spondylitis. One of the paradoxical side effects of TNF inhibitors is the development of new onset psoriasis.
If a patient develops TNF-inhibitor induced psoriasis and the patient’s underlying condition is responding well to the TNF inhibitor, then efforts should be made to keep the patient on this medication and try to control the psoriasis using topical therapies, phototherapy, or traditional systemic medications such as methotrexate or cyclosporine, depending on the severity of the psoriasis. If these measures are ineffective, then it may be worth switching to another class of medication.